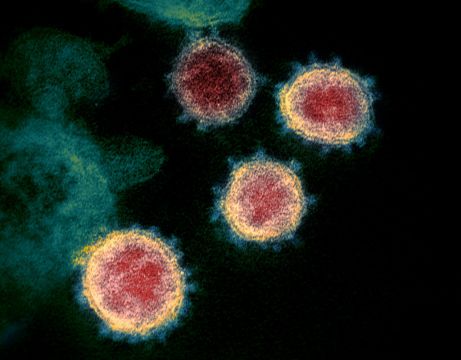
Researchers have identified differences in DNA that may explain why some people get more severely ill from the coronavirus.
They also now know more about the virus than other conditions routinely seen in hospitals, such as sepsis and flu.
The world’s largest study of the genes involved in critical Covid-19 included more than 57,000 people.
It identified 16 new genetic variants – differences in DNA – associated with severe Covid-19, including some related to blood clotting, immune response and inflammation.
Experts suggest the findings open up new fields of research focused on potential new treatments and more accurate diagnosis.
Professor Kenneth Baillie, the project’s chief investigator and a consultant in critical care medicine at University of Edinburgh, said: “Our latest findings point to specific molecular targets in critical Covid-19.
“These results explain why some people develop life-threatening Covid-19, while others get no symptoms at all.
“But more importantly, this gives us a deep understanding of the process of disease and is a big step forward in finding more effective treatments.
“It is now true to say that we understand the mechanisms of Covid better than the other syndromes we treat in intensive care in normal times – sepsis, flu, and other forms of critical illness.
“Covid-19 is showing us the way to tackle those problems in the future.”
Novel gene variants
Professor Mark Caulfield from Queen Mary University of London, formerly chief scientist at Genomics England and co-author on the study, said: “As Covid-19 evolves, we need to focus on reducing the number of people getting seriously ill and being hospitalised.
“Through our whole genome sequencing research, we’ve discovered novel gene variants that predispose people to severe illness – which now offer a route to new tests and treatments, to help protect the public and the NHS from this virus.”
The findings are published in the Nature journal.
Prof Baillie added: “On sepsis and flu, one of the driving forces behind the study is tackling those problems.
“The 120 clinical trials that have been done in sepsis and of immunomodulatory therapy – drugs that target the immune system to try to stop it from causing organ damage, and all of them failed.
“I think that’s a hypothesis test of the question ‘do we understand the biology of sepsis?’.
“And I think the answer is emphatically that we don’t.”
He added that researchers will continue to look to tackle the problems of sepsis and flu, and that it is hoped there might be some clinical impact on sepsis within the next 10 years.
Prof Caulfield said: “This is a really important study, because today we extend the role of whole genome sequencing for rare disease and cancer – which is already in our NHS – to infectious disease, and how we as humans respond to exposure to the virus that none of us knew about two and a half years ago.
“This is a major finding. It’s a major extension of genomics, and we found a lot of things for a relatively modest sample size.”
Intensive care patients
Researchers from the GenOMICC consortium – a global collaboration to study genetics in critical illness – led by University of Edinburgh in partnership with Genomics England, made the discoveries by sequencing the genomes of 7,491 patients from 224 intensive care units in the UK.
Their DNA was compared with 48,400 other people who had not had coronavirus, and that of a further 1,630 people who had experienced mild Covid.
The findings included how a single gene variant was enough to increase a patient’s risk of severe disease, and suggests a specific treatment may help manage disease in the early stages.
According to the researchers, not everyone will have all the DNA changes they identified and therefore some people will have a greater or lesser tendency to have severe outcomes.
Prof Caulfield explained: “I think what we can say today is that these variants do denote people that are more likely to have a critical illness.
“And if we knew about them earlier in the course of their illness, we might be able to consider early intervention with some of the medicines we’ve been talking about, such as dexamethasone or others to try and prevent an adverse outcome.”
However, the experts suggest that while doctors might be able to make predictions about patients based on their genome, the technology is not there yet.
Prof Baillie said: “I think most clinicians would tell you that it was completely bewildering the first time we saw patients with this disease because we’ve never seen it before.
“And there was a really palpable sense that we didn’t understand it and we didn’t know what to do.
“And now you have three effective treatments to suppress people’s immune response and 23, in total, robust genetic associations with identifying the mechanisms of disease – an extraordinary rate of progress.”